Hypothyroidism up to date8/12/2023 Consensus was achieved for all recommendations by the task force. Stakeholder input was received at a national meeting, with some subsequent refinement of the clinical questions addressed in the document. The final document was organized so that each topic is introduced with a question, followed by a formal clinical recommendation. For clinical recommendations, the supporting evidence was appraised, and the strength of each clinical recommendation was assessed, using the American College of Physicians system. When responses were not suitable for a formal clinical recommendation, a summary response statement without a formal clinical recommendation was developed. The responses to questions were formatted, when possible, in the form of a formal clinical recommendation statement. Ethics reviews were provided, when relevant, by a bioethicist. Clinical reviews were supplemented, when relevant, with related mechanistic and bench research literature reviews, performed by our team of translational scientists. The clinical literature relating to each question was then reviewed. Methods: Task force members identified 24 questions relevant to the treatment of hypothyroidism. This document is intended to inform clinical decision-making on thyroid hormone replacement therapy it is not a replacement for individualized clinical judgment. 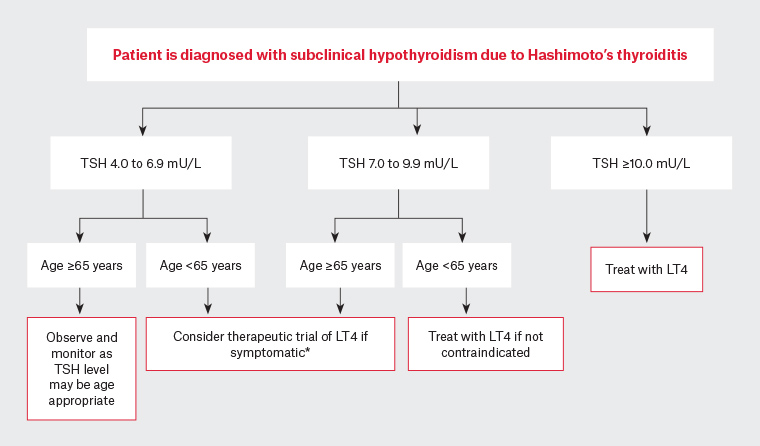
We wished to determine whether there are sufficient new data generated by well-designed studies to provide reason to pursue such therapies and change the current standard of care. 
The purpose of this task force was to review the goals of levothyroxine therapy, the optimal prescription of conventional levothyroxine therapy, the sources of dissatisfaction with levothyroxine therapy, the evidence on treatment alternatives, and the relevant knowledge gaps. An algorithm for a correct approach of these disorders when linked is also provided.Background: A number of recent advances in our understanding of thyroid physiology may shed light on why some patients feel unwell while taking levothyroxine monotherapy. We also discuss the major causes of failure to achieve an optimal management of thyroid dysfunction in diabetic patients and provide recommendations for assessing and treating these disorders during therapy with antidiabetic drugs. 
Therefore, we offer recommendations for the diagnosis, management, and screening of thyroid disorders in patients with diabetes mellitus, including the treatment of diabetic patients planning a pregnancy. An untreated thyroid dysfunction can impair the metabolic control of diabetic patients, and this association can have important repercussions on the outcome of both of these disorders. We also elucidate the common susceptibility genes and the pathogenetic mechanisms contributing to the autoimmune mechanism involved in the onset of type 1 diabetes mellitus and autoimmune thyroid disorders. We assess the current state of knowledge on the central and peripheral control of thyroid hormone on food intake and glucose and lipid metabolism in target tissues (such as liver, white and brown adipose tissue, pancreatic β cells, and skeletal muscle) to explain the mechanism linking overt and subclinical hypothyroidism to type 2 diabetes and metabolic syndrome. This review critically discusses the different underlying mechanisms linking type 1 and 2 diabetes and thyroid dysfunction to demonstrate that the association of these two common disorders is unlikely a simple coincidence. Several studies have documented the increased prevalence of thyroid disorders in patients with diabetes mellitus and vice versa. Thyroid dysfunction and diabetes mellitus are closely linked.
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
